Your jawbone does more than hold your teeth — it shapes your face, allows you to chew and speak properly, and supports your long-term oral health. When the jawbone weakens or shrinks, it can lead to tooth loss, changes in facial structure, and more complex, costly treatments in the future.
You will learn what keeps your jawbone strong, what causes bone loss, and which preventive steps and treatments can help protect or rebuild it. If you notice early warning signs such as loose teeth or receding gums, visiting a trusted dental clinic in Honolulu can help you address bone loss before it progresses. This guide will help you understand your options so you can keep your mouth functional and your facial structure healthy for years to come.
Understanding Jawbone Health
Your jawbone supports your teeth, shapes your face, and helps you bite and speak. Problems can change how you look, what you can eat, and how well dental work like implants will hold.
What Is Jawbone Health?
Jawbone health means the strength and structure of the mandible (lower jaw) and maxilla (upper jaw) that hold your teeth. Healthy jawbone has dense alveolar bone around each tooth root. That bone adapts to chew forces and keeps teeth stable.
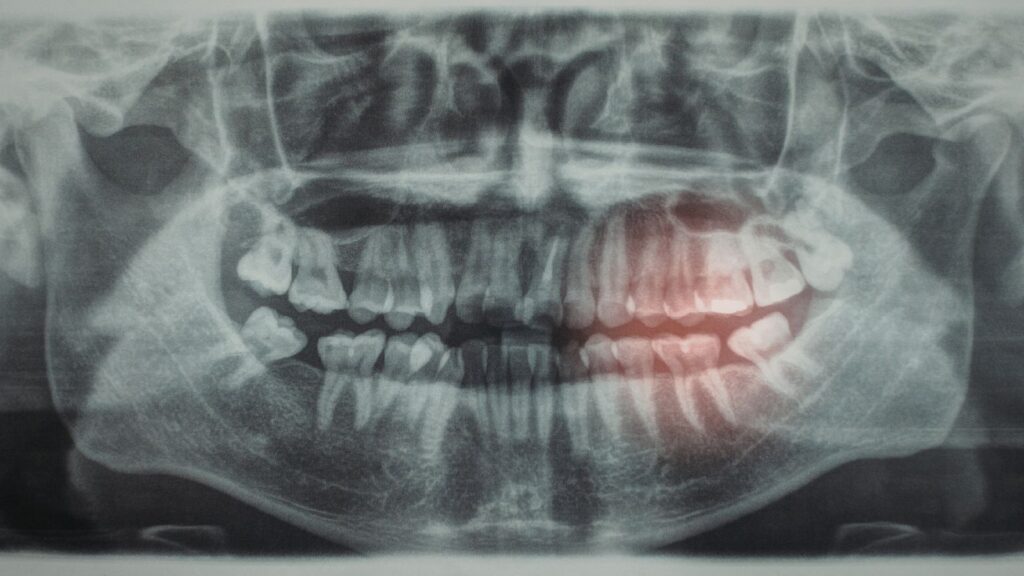
Bone needs regular stimulation from chewing and healthy blood flow to stay strong. Losing teeth, long-term denture use, infection, or some medical conditions can cause the bone to shrink. Dentists measure bone height and density with X-rays to check how much bone you have.
Key Functions of the Jawbone
The jawbone anchors every tooth and transfers chewing forces to the skull. It keeps teeth aligned so you can bite, grind, and chew without pain. It also helps shape your lower face and jawline, which affects your appearance.
Beyond chewing, the jawbone supports speech by holding the teeth that shape sounds. It protects nerves and blood vessels that run through the jaw. Strong bone makes dental treatments like bridges and implants possible. When bone weakens, you may need grafts or other procedures to restore support.
Signs of Jawbone Problems
Watch for loose teeth, changes in bite, or teeth that shift position. These often mean the bone around the roots has decreased. You might also feel pain or swelling around a tooth, which can signal infection and bone loss.
Other signs include difficulty chewing hard foods, a sunken lower face, or ill-fitting dentures. Chronic jaw pain, clicking, or limited mouth opening can point to joint or bone issues. Your dentist can confirm problems with dental X-rays or a CT scan and recommend treatment.
Why Jawbone Health Is Essential to Overall Wellness
Good jawbone health supports your teeth, keeps your face shape stable, and links to other body systems. The next parts explain how bone loss affects chewing, appearance, and overall health.
Impact on Oral Health
Your jawbone holds your teeth in place. When bone shrinks after tooth loss or infection, neighboring teeth can loosen or shift. That makes chewing harder and raises your risk of cavities and gum disease.
Dentists use X-rays to check bone height and density. Early signs include a change in bite, loose teeth, or increased sensitivity. Treatments like bone grafts or implants can rebuild support so you can chew comfortably again.
Keep your jawbone strong by treating infections fast, replacing missing teeth on time, and following dentist advice for cleaning and regular checkups.
Influence on Facial Structure
The jawbone shapes your lower face. When bone volume drops, your cheeks and lips lose support. That can cause a collapsed bite, deeper folds around the mouth, and a shorter appearance between nose and chin.
Bone loss after tooth removal can be fast in the first year. Restoring bone with grafts or placing implants helps preserve natural contours. Small changes in bone height change how your jaw fits together and how your smile looks.
If you want to keep a natural face shape, talk to your dentist about options soon after tooth loss rather than waiting for more bone to disappear.
Connection Between Jawbone and Systemic Health
Jawbone problems can reflect or affect wider health. Chronic oral infections like periodontitis release bacteria and inflammation into the bloodstream. That links to higher risk for diabetes complications, heart disease, and poor healing.
Low bone density in the jaw can also signal general bone loss from osteoporosis. Your dentist may spot these signs before other doctors. Treating oral inflammation and checking calcium or vitamin D can help both jaw and body health.
Tell your dentist about chronic conditions and medications. Coordinating care helps manage risks and keeps both your mouth and body healthier.
Factors Affecting Jawbone Health
Several clear factors change how strong your jawbone stays: what you eat, medical conditions that affect bone, and dental treatments that remove or replace teeth. Each factor can speed up or slow bone loss and change how your face looks and works.
Role of Nutrition
Your jawbone needs minerals and protein to stay dense and heal after injury. Calcium and vitamin D are essential; without them, bone remodeling slows and you may lose bone mass. Aim for foods like low-fat dairy, leafy greens, canned salmon with bones, and fortified cereals. Get about 600–800 IU of vitamin D from diet and sunlight, more if a doctor prescribes it.
Protein supports bone matrix and repair. If you eat little protein, your body can’t rebuild bone well. Avoid very high soda or sugar intake; these can harm bone indirectly by displacing healthier foods and worsening gum disease. If you take supplements, follow a provider’s advice to avoid excess calcium or vitamin D.
Common Medical Conditions
Certain diseases speed jawbone loss by changing bone metabolism or causing inflammation. Osteoporosis lowers bone density bodywide and raises risk of jaw thinning. Diabetes, when poorly controlled, increases infection risk and slows healing after extractions or implants. Periodontal (gum) disease causes local inflammation that erodes the alveolar bone around teeth.
Medications matter too. Long-term steroid use weakens bone. Some cancer drugs and antiresorptive drugs (used for osteoporosis) can rarely affect jaw healing; discuss risks with your dentist before extractions. Smoking lowers blood flow, reduces healing, and raises infection risk, so quitting helps protect your jawbone.
Dental Procedures and Their Effects
Tooth loss causes the nearby jawbone to shrink because it no longer gets chewing forces. After a tooth extraction, the alveolar ridge can resorb quickly in the first year. Dental implants replace a tooth root and stimulate bone if placed properly, which helps stop resorption.
Bone grafts and ridge preservation at time of extraction can maintain height and width for future implants. Poorly fitting dentures can speed bone loss by concentrating pressure on certain areas. If you need extractions, implants, or dentures, plan with your dentist about timing, bone grafting, and smoking cessation to protect long-term jawbone health.
Protecting and Improving Jawbone Health
You can protect your jawbone by stopping damage early, choosing habits that strengthen bone, and using modern dental treatments when needed. Small daily actions and timely care make the biggest difference.
Preventative Dental Care
Keep any dental appointments for cleanings and exams at least every six months, or more often if your dentist recommends it. Professional cleanings remove plaque and tartar that cause gum disease, the main driver of jawbone loss.
Brush twice a day with fluoride toothpaste and floss daily to cut bacterial buildup near the tooth roots. Use an interdental brush or water flosser if you have wide spaces or implants.
If you lose a tooth, act quickly. Ask your dentist about immediate options like temporary prosthetics and a plan for long-term replacement. Early replacement helps keep the alveolar bone stimulated and slows resorption.
Tell your dentist about past extractions, gum infections, or chronic conditions like diabetes. Those raise your risk of bone loss and may require targeted monitoring or earlier X-rays.
Healthy Lifestyle Choices
Eat a balanced diet that supplies calcium, vitamin D, and protein to support bone maintenance. Good sources include low-fat dairy, leafy greens, fatty fish, and lean meats.
Stop smoking and limit heavy alcohol use. Both weaken bone healing and raise your risk for periodontal disease and implant failure.
Maintain regular physical activity, especially weight-bearing exercise, to support overall bone health. While jawbone responds mainly to chewing forces, systemic bone health helps recovery after dental procedures.
Control chronic conditions such as diabetes and osteoporosis. Manage blood sugar and follow your doctor’s treatment plan; this lowers infection risk and improves healing after dental work.
Modern Treatment Options
Dental implants replace missing teeth and stimulate the jawbone much like natural roots. Implants preserve bone height and facial shape when placed by a qualified clinician.
Bone grafting rebuilds lost jawbone for implants or to restore contour. Your dentist may use your own bone, donor bone, or synthetic materials. Grafting success depends on good oral hygiene and overall health.
Guided tissue regeneration and sinus lifts target specific areas of bone loss in the upper jaw. These procedures create space and support for bone to regenerate before implant placement.
If gum disease has advanced, scaling and root planing, plus antibiotics or laser therapy, can halt infection and protect remaining bone. Discuss risks, costs, and recovery time with your dental team to choose the best option for your situation.
Bob Duncan is the lead writer and partner on ConversationsWithBianca.com. A passionate parent, he’s always excited to dive into the conversation about anything from parenting, food & drink, travel, to gifts & more!

